If you spend any time reading about neurofeedback online, you will find two versions of reality. One claims neurofeedback fixes everything from ADHD to trauma to chronic pain. The other dismisses it as expensive placebo. Neither version is accurate. The research paints a more nuanced picture, and clinicians considering this modality deserve to see it clearly.
I am studying for BCIA and IQCB board certification and using neurofeedback in my clinical practice. Here is what I have found when I went past the marketing and into the peer-reviewed literature.
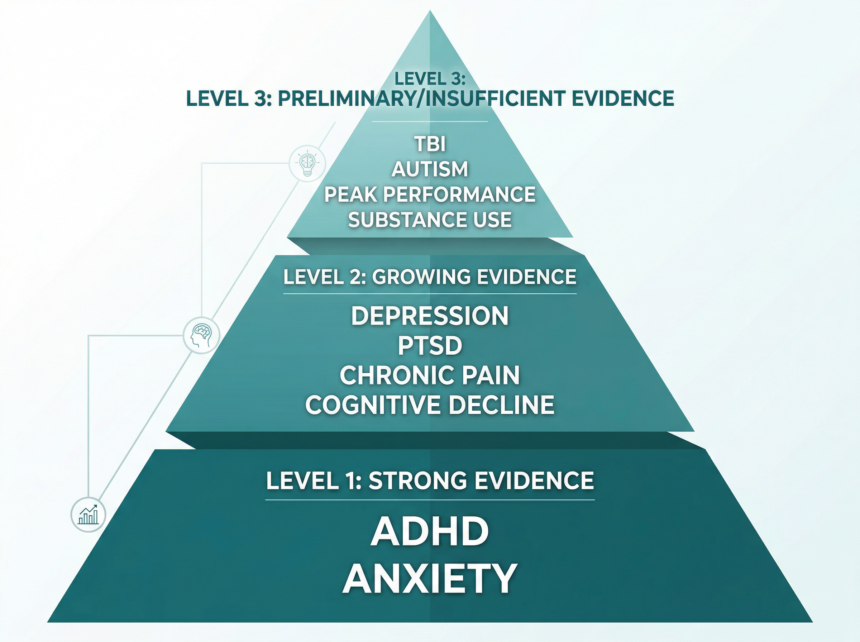
Where the Evidence Is Strongest
Two conditions have the most developed research base for neurofeedback in clinical mental health practice. Neither shows neurofeedback as a standalone cure. Both show meaningful, measurable effects when used alongside other treatments.
ADHD
ADHD neurofeedback research is extensive. The Cortese et al. (2016) Cochrane meta-analysis of 24 RCTs found moderate effect sizes for inattention (d = 0.58) and smaller effects for hyperactivity (d = 0.46). Theta/beta ratio training is the most studied protocol, with effect sizes ranging from d = 0.5 to 1.2 depending on the outcome measure (Arns et al., 2020).
Here is where it gets honest. A well-designed double-blind sham-controlled trial by Gelade et al. (2018, published in Lancet Psychiatry, N = 104) found that real neurofeedback was not significantly better than sham on the primary outcome measure. The difference between groups was d = 0.39. That suggests real effects exist, but a substantial portion of the benefit (an estimated 30 to 50 percent) may come from placebo and expectancy.
The AACAP does not recommend neurofeedback as first-line treatment for ADHD. It is considered potentially acceptable as an adjunct to established treatments in children and adolescents with adequate access and willingness. That framing matters. “Adjunct” is different from “alternative.”
The International Society for Neurofeedback and Research (ISNR) rates ADHD neurofeedback at Level 3 (Probably Efficacious). That is a meaningful designation, but it is one level below the strongest classification.
Anxiety
Anxiety disorders show moderate-to-strong evidence for neurofeedback, with effect sizes in the d = 0.5 to 0.8 range across several protocols. A 2021 RCT by Warncke et al. (N = 42) found a 35 percent reduction in GAD-7 scores for real neurofeedback versus 15 percent for sham (d = 0.71), with effects sustained at six-month follow-up.
The mechanism is clear: neurofeedback targeting emotion regulation circuitry (amygdala, anterior cingulate, insula) directly modulates the neural systems involved in anxiety. Real-time fMRI studies show corresponding changes in brain activation patterns.
The ADAA recognizes neurofeedback as a promising adjunctive approach but considers the evidence insufficient for monotherapy. Helpful alongside other treatments, not a replacement for them.
Where the Evidence Is Growing
Several conditions show promising results that are building toward clinical relevance. The research is not yet as deep as ADHD or anxiety, but there is enough here to inform your clinical thinking.
Depression: A meta-analysis by Linhartova et al. (2019, 10 studies, N = 223) found a mean effect size of d = 0.74 for neurofeedback targeting depression-related brain circuits. Heterogeneity was high, only three studies were RCTs, and most were underpowered. Combined EEG protocols (alpha/theta) paired with mood induction show moderate effects (d = 0.5 to 0.7), but active control comparisons are still lacking. The ISNR rates depression neurofeedback at Level 2 (Possibly Efficacious).
PTSD: Small studies (N = 10 to 30) show symptom reductions when neurofeedback targets amygdala reactivity and prefrontal regulation. A systematic review by Nicholson et al. (2020) found effect sizes ranging from d = 0.3 to 1.1, but only one study included a proper control group. No study has demonstrated superiority to established trauma treatments like Prolonged Exposure or CPT. For clinicians already doing trauma work, neurofeedback is a plausible adjunct, but the evidence base is still thin compared to first-line treatments.
Chronic pain: A 2013 RCT by Jensen et al. (N = 68) found 25 percent pain intensity reduction with real neurofeedback versus 10 percent with sham (d = 0.72), sustained at three months. Multiple studies converge on similar moderate effects. The research here is more methodologically rigorous than in some other emerging areas, but still limited in sample size.
Cognitive decline: Neurofeedback for mild cognitive impairment (MCI), early-stage Alzheimer’s, and post-stroke cognitive rehabilitation is an active area of research. Several small studies show improvements in attention, memory, and processing speed when targeting alpha and theta band activity. A 2020 systematic review identified moderate effect sizes (d = 0.4 to 0.7) across cognitive outcomes in aging populations, though sample sizes remain small (typically N = 15 to 40) and few studies include adequate control conditions. This is worth watching for clinicians who see older adults, but not yet established enough for clinical claims.
Sleep disorders: Some evidence supports sleep spindle enhancement training for insomnia, with effect sizes around d = 0.5 to 0.7. CBT for insomnia remains the gold standard with substantially larger effect sizes (d = 0.9 to 1.4).
Where the Evidence Is Thin – for now
Some conditions frequently associated with neurofeedback in popular media have very limited research support:
- Peak performance / cognitive enhancement: Peer-reviewed studies show 1 to 5 percent improvements at best. Commercial claims of 10 to 20 percent gains are not supported. However, a more regulated brain, is a more regulated brain.
- Traumatic brain injury: Mostly case reports. Natural recovery in the first six months post-injury confounds any apparent treatment effect.
- Autism spectrum: No adequately powered RCTs. Case series with small samples and heterogeneous outcomes.
- Substance use disorders: Pilot studies show some promise for reduced craving and improved adherence, but dropout rates exceed 50 percent and no controlled trials exist.
These are areas where the research question is valid but the data is not yet sufficient to guide clinical practice.
A note on epilepsy: the seizure research is actually some of the strongest in the entire neurofeedback literature. Sensorimotor rhythm training for drug-resistant epilepsy has been endorsed by the American Epilepsy Society, and the ISNR rates it at their highest evidence level. Most clinicians in private mental health practice will not be treating seizure disorders directly, but the epilepsy research matters because it demonstrates that the mechanism of neurofeedback is real and measurable. The brain can learn to change its own electrical patterns through operant conditioning. That foundational finding supports everything else in this field.
How Neurofeedback Works (Briefly)
Neurofeedback applies operant conditioning to brain activity. A client receives real-time visual or auditory feedback about their brainwave patterns. When the brain produces patterns closer to the training target, the client receives a reinforcing signal. Over repeated sessions, the brain learns to produce those patterns more reliably.
The mechanism draws on neuroplasticity. Repeated engagement of specific neural circuits, coupled with feedback about success, drives synaptic and potentially structural changes. Research shows that successful neurofeedback training strengthens functional connectivity between volitional control regions (primarily dorsolateral prefrontal cortex) and the target regions being trained.
This is not mysterious. It is operant conditioning applied to a biological system, producing measurable neurophysiological changes. The question is not whether the mechanism is real. The question is how large the clinical effect is for each condition and how much of what we observe in studies is driven by the training itself versus expectancy.
What Clinicians Should Take Away
Neurofeedback is a real modality with real effects. The evidence for ADHD and anxiety is moderate to strong. Depression, PTSD, chronic pain, and cognitive decline are growing areas with promising early data. Several other conditions need more rigorous trials.
Effect sizes are modest. Across most conditions, expect effect sizes in the d = 0.4 to 0.8 range. That is clinically meaningful. It is not miraculous.
Placebo and expectancy are real factors. Sham-controlled studies consistently show that a meaningful portion of neurofeedback benefit comes from the therapeutic relationship, client expectations, and the experience of receiving treatment. Honest expectation-setting with clients is essential.
Neurofeedback works best as part of a comprehensive approach. No evidence supports neurofeedback as a standalone replacement for established treatments. The conditions where it shows the most benefit are those where it supplements psychotherapy, medication, or other standard care.
Responder variability is high. Roughly 40 to 60 percent of individuals show meaningful benefit across well-studied conditions. The field does not yet have reliable ways to predict who will respond, though QEEG-informed protocol selection is a promising direction.
The research is improving. More studies are using active controls, sham conditions, and adequate sample sizes than a decade ago. The evidence base will look different in five years. That is worth tracking.
For clinicians considering neurofeedback training, the research supports adding it to your clinical toolkit. It does not support promising clients outcomes the literature cannot deliver. Knowing the difference is part of being competent in this field.
Leave a Reply